Ours is a holistic approach that does not hinder the physiological processes of the body. It's an approach that encourages the restoration of balance, by combatting the causes of symptoms as efficiently as possible and ensuring fast relief.
Symptoms and relief
SELECT YOUR NEED

Food intolerances
WHAT ARE FOOD INTOLERANCES?
Food intolerances, in the strict sense of the word, are adverse reactions to food resulting from the body having difficulty metabolizing a given food or food component. They do not involve the immune system directly and have various causes, including, for example, an enzyme deficiency.
What is commonly referred to as food intolerance (e.g., to pork, apples, tomatoes, etc.) is an IgG-mediated adverse reaction to food. Unlike allergies, it is a problem that can be reversed through a balanced and responsible lifestyle that involves a functional and targeted diet, first eliminating that particular food and then reintegrating it. In this type of adverse reaction, the body's response is slower (1 to 36 hours) than in (IgE mediated) food allergies, which induce a near-immediate reaction.

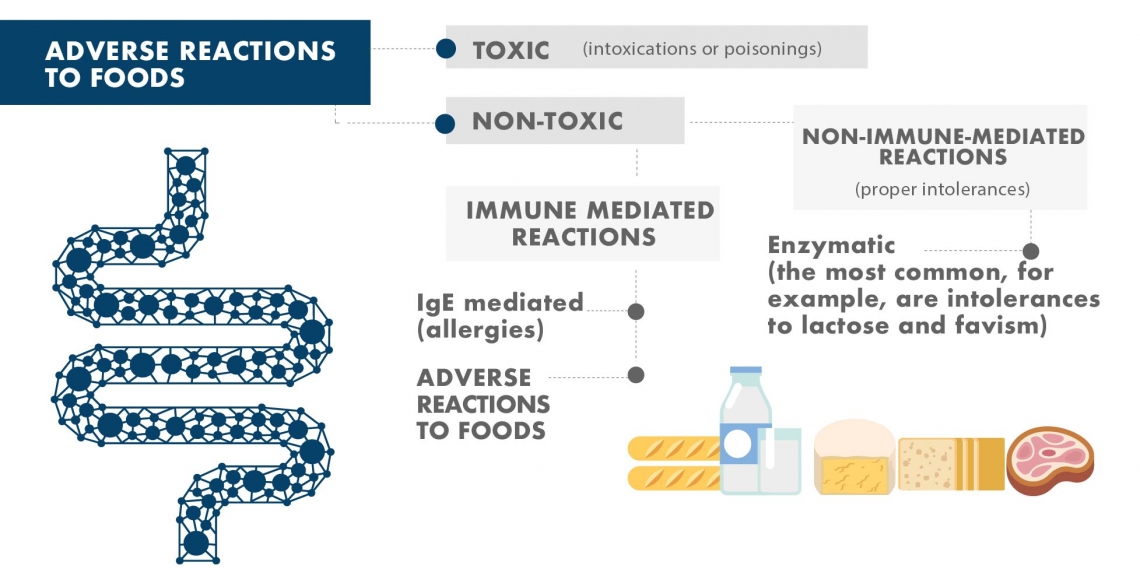
WHY IT IS USEFUL TO INVESTIGATE THE DEGREE OF TOLERANCE TO FOOD ANTIGENS
There are disorders and symptoms that can have very different causes. Most of these symptoms are warning signals sent out by our intestines and are an expression of an overreaction that occurs after consuming a given food.
Today there are so many people, both children and adults, who may exhibit altered tolerance to certain food antigens, most often without being aware of it: THE INCIDENCE IS ABOUT 40% of the population.

The new therapeutic frontiers are not limited solely to recommending products to control the symptom, but are geared towards investigating the root causes.
WHAT ARE THE CAUSES OF IGG-MEDIATED ADVERSE REACTIONS TO FOODS?
The main cause can certainly be found at the level of the digestive tract, which is a gateway for a wide range of antigens. The adverse reaction to these antigens seems to be the direct consequence of a condition of dysbiosis and of an intestinal mucosa which has lost its integrity for a variety of possible causes.
CAUSES OF THE ALTERATION OF THE INTESTINAL MUCOSA
- stress
- unhealthy diet and lifestyle
- intestinal dysbiosis
- exposure to environmental toxins
- chronic inflammation
- infections and frequent use of medications
- low or excessive physical activity
- lack of nighttime rest
- cigarette smoke

WHAT ARE THE SYMPTOMS OF IGG-MEDIATED ADVERSE REACTIONS TO FOODS?
Adverse reactions to foods produce a range of disorders, both within the intestine and outside of it
- GASTRO-INTESTINAL
abdominal bloating, meteorism, digestive difficulties, diarrhea, nausea, constipation, colitis, intestinal inflammation, belching - GENITO-URINARY
cystitis, vaginitis, candida, dysmenorrhea, enuresis, chronic cystitis - DERMATOLOGICAL
itching, acne, eczema, atopic dermatitis, hives, psoriasis - RESPIRATORY
sinusitis, bronchitis, rhinitis, excessive expectoration, asthma, otitis, nasal congestion - MUSCULOSKELETAL
muscle aches, muscle cramps, osteoarticular pain - NEUROLOGICAL
headaches, fatigue, mood swings, hyperactivity, asthenia, brain fog, poor concentration, sleep disturbances - GENERAL
weight gain, obesity, water retention and a sensation of heaviness
Prodeco Pharma offers PRODIAGNOSIS FOOD TOLERANCE 92 foods and PRODIAGNOSIS FOOD TOLERANCE DISBIOSI for the investigation of adverse reactions to foods
PRODIAGNOSIS FOOD TOLERANCE 92 foods
If PRODIAGNOSIS FOOD TOLERANCE 92 detects a loss of food tolerance, the bacterial flora is likely out of balance, and the intestinal mucosa is inflamed and not performing its barrier function optimally. Recognizing foods that are not tolerated gives you the opportunity to create a customized diet that involves an initial, temporary discontinuation of the food, followed by a gradual, slow reintroduction. The benefits are regression of disorders and inflammatory processes, recovery of food tolerance, and well-being of the digestive system and the body as a whole.
Testing method: capillary self-sampling.


PRODIAGNOSIS FOOD TOLERANCE DISBIOSI
FOOD TOLERANCE 92 differs in that it expands the search for predisposing factors for loss of food tolerance by investigating the status of intestinal bacterial flora. The combination of information derived from the presence of IgG in the blood and specific elements released in the urine (indacane and scatol) allows specific recommendations to be given, also aimed at restoring the balance of the intestinal flora, the impairment of which (dysbiosis) may be concomitant to the loss of gut wall integrity and adverse reactions to food.
Testing method: urine and capillary self-sampling.
WHAT DO WE OFFER?
- RELIABLE AND REPRODUCIBLE RESULTS USING THE LATEST INNOVATIVE DIAGNOSTIC TECHNIQUE WITH HIGH SPECIFICITY AND SENSITIVITY (MICROARRAY)
- EVALUATION OF TEST RESULTS BY AN EXPERT GASTROENTEROLOGIST NUTRITION DOCTOR with many years of experience in the field of gastrointestinal disorders
- TEST REPORT
- REPORT with SPECIFIC FOOD RECOMMENDATIONS FOR SUSPENSION AND SUCCESSFUL REINTEGRATION OF THE INDIVIDUAL FOODS to which the adverse reaction arose
- IN THE REPORT, A SCHEMATIC TABLE WILL BE INCLUDED with the list of supplements useful for the symptoms indicated in the questionnaire, which will be filled out with the pharmacist or herbalist at the point of sale offering the PRODIAGNOSIS service
- HIGH QUALITY AND PROFESSIONAL SERVICE INTEGRATED with pharmacies, parapharmacies and herbalists that promote the values of Prodeco Pharma by also making the PRODIAGNOSIS service available.
IN ORDER TO CARRY OUT THE TEST, CONTACT THE POINT OF SALE (PHARMACY OR HERBALIST SHOP) AFFILIATED WITH THE PRODIAGNOSIS SERVICE

DO YOU KNOW THE DIFFERENCE BETWEEN AN ALLERGY, INTOLERANCE AND ADVERSE REACTION TO FOOD?
Since these are complex topics that are sometimes presented in a misleading manner, we will describe what allergy, intolerance, and adverse reaction to food are and the testing methods to detect each of them.
ALLERGY: arises from the immune system, which recognizes a protein component in food as potentially harmful and produces IgE antibodies, triggering an instantaneous allergic reaction that typically manifests as hives, oral allergy syndrome and, in extreme cases, anaphylactic shock.
- A diagnosis of allergy requires specific tests such as the Prick test, RAST, Prick by Prick, Patch test, Prist and trigger tests.
INTOLERANCE: Does NOT arise from the body's immune system. Intolerances are due to an enzyme defect. The most common are lactose intolerance and favism.
- The diagnosis of lactose intolerance is made with specific tests such as the Lactose Breath Test.
- The diagnosis of favism requires specific tests such as peripheral smear and the glucose-6-phosphate dehydrogenase (G6PD) procedure.
IgG-MEDIATED ADVERSE REACTION TO FOOD: This involves the production of IgG antibodies by the immune system that interact with certain protein components in the food, resulting in a loss of tolerance towards the food by the body. In adverse reactions to food, often incorrectly called intolerances, the body's response is slower than in allergies: it occurs from 1 to 36 hours after food consumption and causes less severe overall symptoms than allergies.
The most common symptoms are bloating, heaviness, digestive difficulty, headache, bad breath, skin rashes, dermatitis, water retention, fatigue, sleep disturbances, diarrhea or constipation.
The discomforts listed above, while significantly affecting the quality of life, can often be warning signs to investigate a loss of tolerance by the body towards foods and start on a path of recovery aimed at restoring well-being. Thus, what is very often referred to as intolerance to pork, apples, tomatoes, milk, etc., is actually an IgG-mediated adverse reaction.
